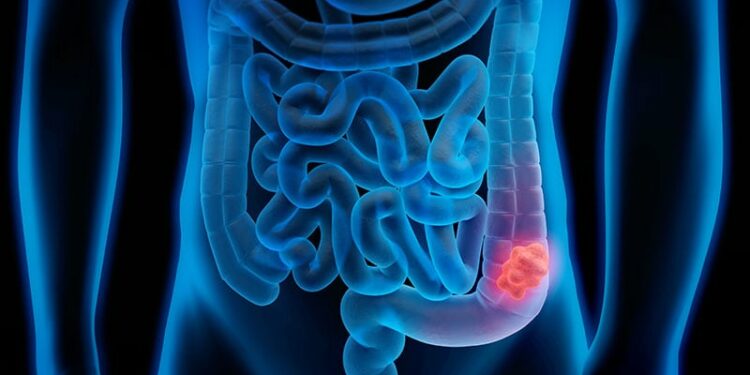
Colorectal cancer (CRC) is a major public health issue, with over 43,000 new cases and nearly 17,700 deaths annually in France. The overall survival rate is currently 63%. It is much higher for early stages than for advanced stages. Screening allows for the diagnosis of the disease in its early stages, when it is responsive to curative treatment, thus reducing specific CRC mortality.
The screening methods currently depend on the risk level of developing CRC, as defined by the Health Authority. Apart from patients at high risk for CRC (eg, those with a personal and family history of polyps or CRC, chronic inflammatory bowel disease, and genetic polyposis), patients aged 50-74 years with average risk are now invited every 2 years to undergo an immunological test detecting human fecal hemoglobin, or FIT. The test has high sensitivity (70%-80%), thus ensuring a good level of detection.
The yield of the test remains low in France, however. It is around 36%, which is below the 45% minimum adherence recommended by the European agency, suggesting a need for other approaches. Hence, the attention given to a new type of blood test that uses cell-free DNA (cfDNA) or circulating free DNA (cfDNA) from circulating blood. Different from tests that use circulating tumor DNA, the new test could improve screening compliance, detect CRC earlier, and reduce mortality.
ECLIPSE Study
Patients who are eligible for CRC screening (those aged 45-84 years without high CRC risk) were included in a prospective, observational, multicenter study across 265 sites in the United States. The study was published in the New England Journal of Medicine. The clinical validation cohort included 10,258 people, of whom 7861 met the eligibility criteria and were evaluable. Overall, 83.1% (54/65) of participants with CRC detected by colonoscopy had a positive cfDNA test, and 16.9% had a negative test, resulting in a sensitivity of 83.1%. The sensitivity for CRC stages I, II, or III was 87.5%, and the sensitivity for advanced polyps (size > 10 mm, villous component, or high-grade dysplasia) was 13.2%.
Overall, 89.6% of participants without colorectal lesions (CRC or advanced polyps, especially serrated) identified during colonoscopy had a negative cfDNA blood test, while 10.4% had a positive cfDNA test, resulting in a specificity of 89.6%. In comparison, the negative colonoscopy specificity was 89.9% (95%).
This study used circulating cfDNA from total blood (also called “liquid biopsy”) to detect alterations, aberrant methylation, and DNA fragment modifications in nearly 7900 participants. The blood test, the composition of which is not fully known, appears to be more effective than its competitor, Septin-9, thus avoiding the need for stool collection.
But the sensitivities of the cfDNA test for CRC and advanced adenomas in this study remain lower than those reported for FIT and a new multitarget fecal DNA (mtfDNA) test, while specificities are similar. In addition, the test’s specificity decreases with age, and its 3-year repetition is not based on scientific evidence.
BLUE-C Study
Another study evaluated a second-generation mtfDNA test with updated DNA biomarkers that had been used in the first-generation test. This study, too, was published in the New England Journal of Medicine. It compared this new test with FIT in more than 20,000 average-risk participants undergoing conventional screening. Although the study did not directly compare the two fecal DNA tests, the new-generation test appears to maintain CRC detection sensitivity (93.9%) and presents improvements in overall specificity for the absence of advanced neoplasia compared with the previous test.
This new fecal test also retained a sensitivity of 43.4% for detecting advanced polyps. The specificity of 90.6% (though still lower than FIT’s specificity, at 94.8%) should increase detection efficiency for users by reducing false-positive results and subsequent colonoscopies.
The Optimal Test
The optimal screening test must meet the following criteria: Satisfactory specificity and sensitivity rates, good patient adherence, low cost, good reproducibility, and low complication risk. While the acceptability of fecal tests is lower than that of blood tests, abnormalities related to CRC and its precursors are more detectable in stool than in blood: Fecal flow carries a continuous stream of exfoliated neoplastic cells in cases of cancer or advanced adenoma. Finally, the timing of colonoscopy relative to the positivity of these two tests remains important, as the COVID-19 pandemic reminds us.
Two editorials complement the analysis of each of the two New England Journal of Medicine articles on the complementary nature of these two innovative approaches. One is diagnostic for invasive CRC screening with a cfDNA blood test named “Shield,” which is awaiting the Food and Drug Administration approval and is already commercially available for around $900. The other is genuinely preventive, based on mtfDNA in stools, and like FIT, raises concerns about acceptability. Their respective costs remain high and are borne by patients.
In conclusion, in an average-risk American population, the cfDNA blood test has a sensitivity of 83% for detecting CRC and a specificity of 90% for advanced neoplasias. However, it seems virtually incapable of detecting advanced polyps, with a sensitivity of only 13%. It therefore serves as an early detection tool for asymptomatic CRC but does not contribute to its prevention.
Prevention still relies on stool use to detect advanced polyps, which are the only true precancerous lesions. The gain from mtfDNA stool testing is thus modest compared with FIT, the gold standard with low cost and high specificity for this indication. To date, some European countries have applied the principle of informed choice for eligible individuals with two jointly proposed screening methods: A screening colonoscopy every 10 years or a biennial FIT followed by a colonoscopy in case of positivity.
However, the best screening test is the one that patients are willing to do, but what about financial coverage?
This story was translated from JIM, which is part of the Medscape professional network, using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
Source link : https://www.medscape.com/viewarticle/can-dna-tests-promote-colorectal-cancer-screening-2024a10007gn?src=rss
Author :
Publish date : 2024-04-18 05:34:48
Copyright for syndicated content belongs to the linked Source.