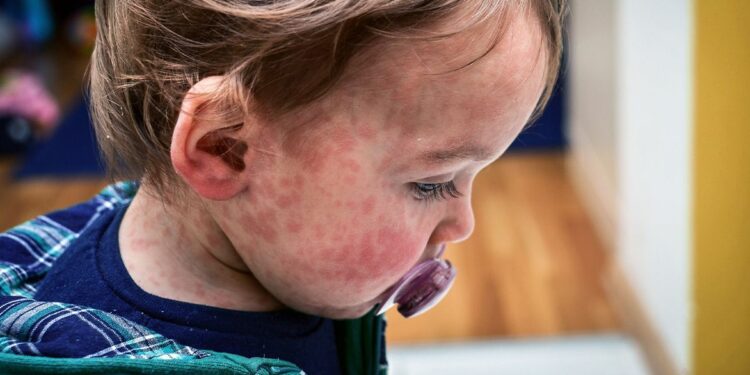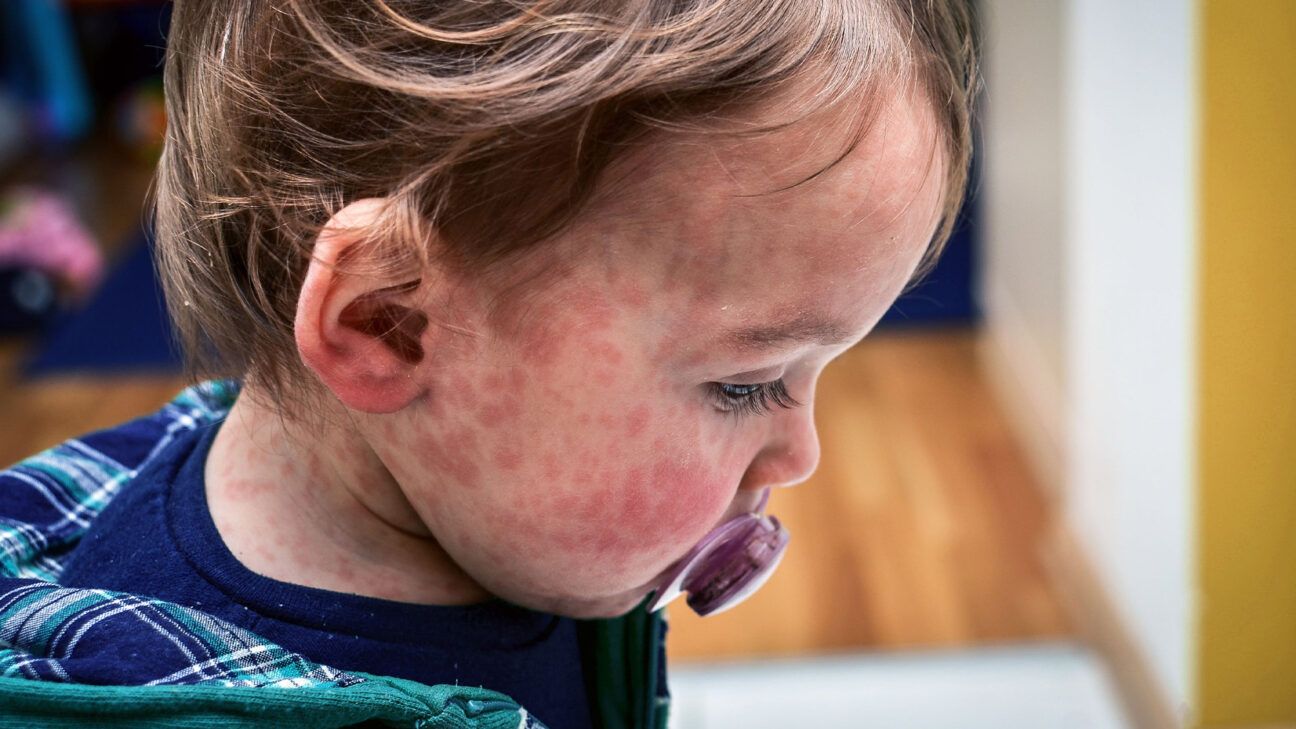
- The CDC issued a health alert on March 18 highlighting the global spread of measles ahead of the busy spring and summer travel season.
- The CDC advises families to vaccinate children as young as 6 months against measles if they plan to travel abroad.
- The American Medical Association echoed the CDC’s warning as childhood vaccine exemption rates reached an all-time high.
Health officials are sounding alarm as rising measles cases in the United States and around the world endanger public health.
The Centers for Disease Control and Prevention (CDC) issued a health alert to physicians on March 18 to draw attention to the global spread of measles ahead of the busy spring and summer travel season.
The CDC noted that many countries affected by recent measles outbreaks are also travel destinations for American tourists, including the United Kingdom, Austria, Romania, and the Philippines.
The agency recommended families traveling abroad with infants as young as 6 months get their child vaccinated against measles a few months ahead of the routine immunization schedule.
Young children usually receive the
Measles outbreaks around the U.S., most recently in Chicago, and those around the world are underscored by low vaccination rates.
The CDC added that measles cases are also brought into the U.S. by travelers who become infected while in other countries.
“As a result, domestic measles outbreaks have been reported in most years, even following the declaration of U.S.
Health experts at the American Medical Association (AMA) echoed the CDC’s warning, urging individuals to get vaccinated against measles prior to travel if they’re not already immune.
“Measles is extremely contagious and can cause life-threatening illness. Vaccination not only prevents infection, measles-related complications and even death, but also helps prevent further spread to loved ones, neighbors, co-workers and others in close contact,” said
Ehrenfeld stressed that when people are not vaccinated against infectious diseases like measles, they put themselves and others at risk of infection, which may lead to severe illness, disability, and even death.
High-risk groups for serious illness from infectious diseases include:
- children too young to be vaccinated
- cancer patients
- immunocompromised people
“The overwhelming scientific evidence shows that vaccines remain among the most effective and safest intervention to both prevent individual illness and protect the health of the public,” Ehrenfeld said.
“The reduction in measles vaccination threatens to erase many years of progress as this previously eliminated vaccine-preventable disease returns.”
The AMA is reminding doctors to talk with their patients about the health risks of not being vaccinated and to continue to make strong recommendations for following immunization schedules unless exemptions are deemed medically inadvisable.
“We also urge physicians to educate patients on the signs and symptoms, severity and complications of measles given that many people are unfamiliar with the impact of the disease,” Ehrenfeld said.
The CDC warning noted as many as 36 states have low childhood vaccination rates.
Fewer than 95% of kindergarten-age children were vaccinated against measles during the 2022–2023 school year, which is below the threshold for herd immunity to prevent community spread.
Herd immunity occurs when a significant portion of the population has some immunity (whether vaccinated or with natural infection) against an infectious disease like measles.
The gap in vaccination coverage has left approximately 250,000 kindergartners at risk for measles infection annually over the past 3 years, according to the CDC.
“The level of immunity to measles in the general population in the U.S. is quite high given high vaccination rates (given in childhood since the 1960s) with high natural infection rates prior to the 1960s,” Dr. Monica Gandhi, MPH, professor of medicine at the University of California, San Francisco, told Healthline.
Population immunity in the U.S. will decline, however, if childhood vaccine rates do not improve, Gandhi warned.
Measles had been declared
But vaccinated individuals or previously infected individuals are
Young children should receive two doses of the measles vaccine, which offers lifetime protection in most cases.
The CDC estimates 97% of people, who have had the recommended two doses of the measles vaccine, are protected against the disease.
Gandhi said some adults may require booster vaccination prior to international travel, prior to college, prior to pregnancy, or during outbreaks.
“The larger population need not be concerned if vaccinations are kept up to date,” Gandhi noted.
Health officials at the CDC and American Medical Association are urging vaccination against measles ahead of the busy spring and travel summer season.
The warning comes as low vaccination rates fuel measles outbreaks in the U.S. and around the world.
While herd immunity against measles remains high in the U.S., this once-eradicated disease puts unvaccinated people and other high-risk groups at risk for infection and severe illness.
Source link : https://www.healthline.com/health-news/cdc-health-alert-measles-vaccine
Author :
Publish date : 2024-03-20 15:55:13
Copyright for syndicated content belongs to the linked Source.